 
They can be frustrating, scary, and dangerous. Sleep attacks are the most obvious symptom of narcolepsy. You may get an uncontrollable feeling of sleepiness beforehand, or it may happen without any warning at all. No matter how much sleep you get overnight, you fall asleep quickly and often during the day. One of the most noticeable symptoms is excessive daytime sleepiness. Narcolepsy is a chronic neurological disorder that stops your brain from regulating your sleep-wake cycles. Your head is on the desk and 10 minutes have passed. The next thing you know, your eyes open and you wake up. Will you grab a burger with co-workers or eat the salad you packed this morning? and you’re sitting at your desk, thinking about lunch. 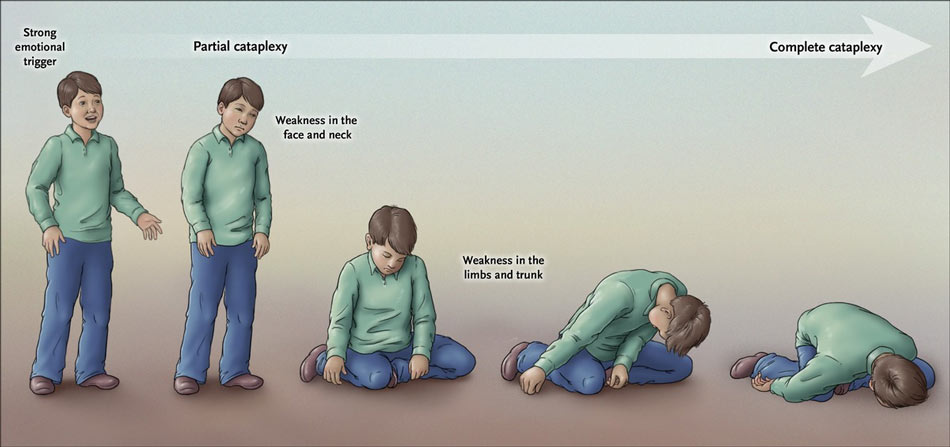
Subcoereulus vlPAG, ventrolateral periaqueductal grey.It’s 11:30 a.m. Medial medulla mPFC, medial prefrontal cortex REM, rapid eye movement SubC, Locus coeruleus LH, lateral hypothalamus LPT, lateral pontine tegmentum MM, Neuronal activity cancels out the inhibitory effect of amygdalar neurons.Ībbreviations: CeA, central amygdala GABA, γ-aminobutyric acid LC, In healthy individuals, orexin-expressing Muscle paralysis inĬataplexy is also enabled by loss of noradrenergic input from LC neurons, whichĪre inhibited during cataplexy. Neuron circuit, triggering muscle paralysis and cataplexy. LC–vlPAG–LPT circuit, which in turn disinhibits the SubC to motor GABAergic CeA neurons inhibit neurons in the The LC–vlPAG–LPTĬircuit normally prevents muscle paralysis during wakefulness by suppressing theĪctivity of SubC neurons. When a positive emotion is experienced, GABAergic neurons in the CeA switch onĪnd inhibit cells in the LC, vlPAG and LPT. 
Neurons in the SubC trigger REM paralysis by activating GABAergic or glycinergicĬells in the MM, which in turn project to and inhibit skeletal motor neurons. Two-part brainstem circuit-the SubC and MM connection. Paralysis is thought to underlie cataplexy, and is probably triggered by a Activation during wakefulness of neural circuits involved in REM sleep Hypothetical circuits and pathways controlling cataplexy in the rodentīrain. This Review describes the clinical and pathophysiological aspects of cataplexy, and outlines optimal therapeutic management strategies. Despite major advances in understanding disease mechanisms in cataplexy, therapeutic management is largely symptomatic, with antidepressants and γ-hydroxybutyrate being the most effective treatments. The amygdala and medial prefrontal cortex contain neural pathways through which positive emotions probably trigger cataplectic attacks. Muscle weakness during cataplexy is caused by decreased excitation of noradrenergic neurons and increased inhibition of skeletal motor neurons by γ-aminobutyric acid-releasing or glycinergic neurons. One pathogenetic mechanism that has been hypothesized for cataplexy is the activation, during wakefulness, of brainstem circuitry that normally induces muscle tone suppression in rapid eye movement sleep. This disorder occurs almost exclusively in patients with depletion of hypothalamic orexin neurons. Occurring spontaneously, cataplexy is typically triggered by strong positive emotions such as laughter and is often underdiagnosed owing to a variable disease course in terms of age of onset, presenting symptoms, triggers, frequency and intensity of attacks. Cataplexy is incapacitating because it leaves the individual awake but temporarily either fully or partially paralyzed. Cataplexy is the pathognomonic symptom of narcolepsy, and is the sudden uncontrollable onset of skeletal muscle paralysis or weakness during wakefulness.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
